Answer
Reduce ventricular sensitivity.
Explanation
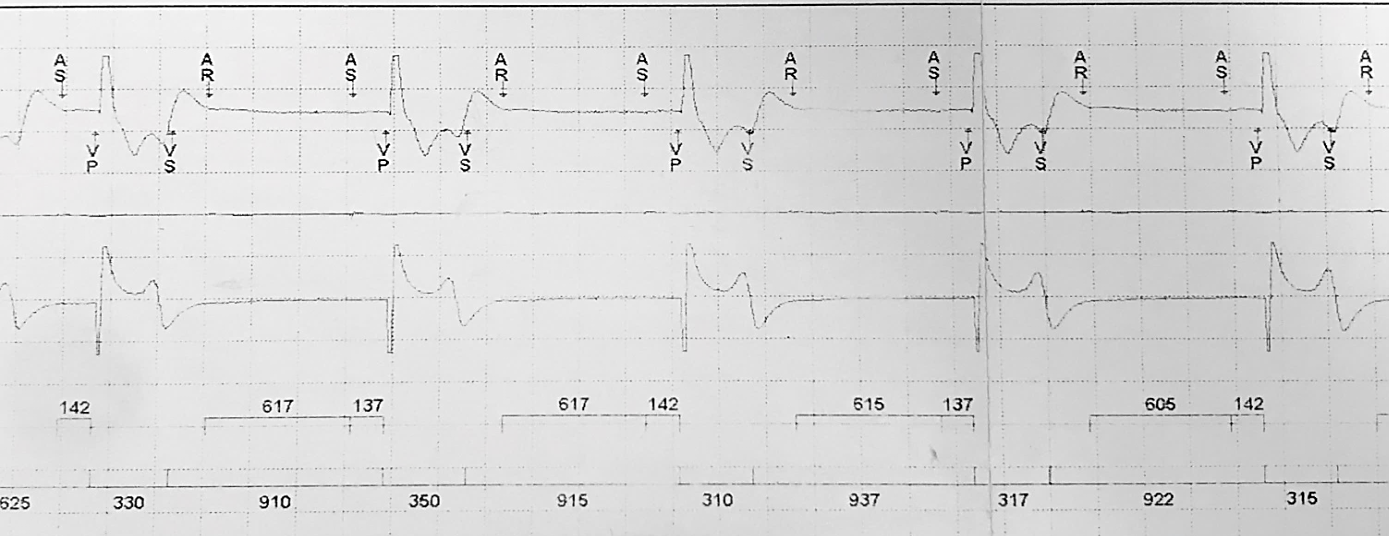
Figure 1 is an example of T Wave oversensing (TWOS) in a patient with hypertrophic obstructive cardiomyopathy. The TWOS is disrupting normal pacemaker function causing functional atrial undersensing and ventricular pacing at a slower rate than the programmed lower rate interval (LRI). The ventricular rate in this EGM is ~ 49 bpm, which during exercise is the reason for the patient’s symptoms.
Reviewing the EGM at the beginning of the trace there is an atrial sense (AS) followed by a ventricular pace (VP) which is appropriate tracking of the intrinsic sinus P wave. The next marker a ventricular sense (VS) clearly lines up with the T wave of the VP beat and is an oversensed T wave. The oversensed T wave (VS marker) triggers a post ventricular atrial blanking period (PVARP) which results in the next sinus P wave being functionally undersensed marked as an atrial refractory (AR) event, which consequently is not tracked and does not trigger a VP. The TWOS also resets the lower rate interval timer which delays the expected next VP and results in pacing occurring at a rate slower than the programmed LRI.
Of the answers available the only programming change to prevent TWOS would be to reduce the ventricular sensitivity (make sensing less sensitive). In this case the ventricular sensitive threshold was increased from 0.9 mV to 1.5 mV which eliminated the T wave over sensing during exercise, illustrated in figure 2.
.png)
Figure 2
EGM recorded during peak exercise post RV sensitivity programming changes. EGM 1 shows the Atrial EGM. EGM 2 RV tip to RV ring EGM and EGM 3 shows Can to RV ring EGM.
Summary
T wave oversensing is commonly encountered in patients with hypertrophic cardiomyopathy and can be seen in patients with long QT, Brugada and hyperkalemia. T wave amplitudes can also vary greatly with changes in posture, autonomic tone and with exercise. In modern ICD systems there are often several device specific algorithms and parameters which can help reduce its occurrence and avoid triggering of inappropriate ICD therapies. In patients with pacemakers TWOS is less commonly observed and there are fewer programming options available. The best by far is to reduce the R wave sensitivity as in this case. Extension of blanking periods when able to or changing the sense vector are also possible programming solutions although are usually less successful.
An interesting point to highlight in this case is the role of exercise testing device patients who present with unexplained exertional symptoms. Although not commonly performed, exercise testing can prove invaluable in the assessment of patient’s symptoms and review of cardiac implantable electronic device (CIED) function.
.png)


.png)