July 2018
Pre-syncope in a dependent pacemaker patient
Sam Griffiths – Senior Cardiac Physiologist
s.griffiths4@rbht.nhs.uk
Background
A 10 year old boy with a CRT-pacemaker implanted for congenital complete heart block attended pacing clinic after an episode of pre-syncope. The pacemaker mode was DDD with a lower rate limit of 80bpm. On interrogation the presenting rhythm was atrial sensing with biventricular pacing (AS/BiVP). The underlying rhythm was complete heart block with no ventricular escape at 30 bpm. All lead measurements were within normal and acceptable ranges and overall there appeared to be normal pacemaker function. There was one EGM captured of a ventricular high rate episode displayed below which happen to correlate to the timing of symptoms.
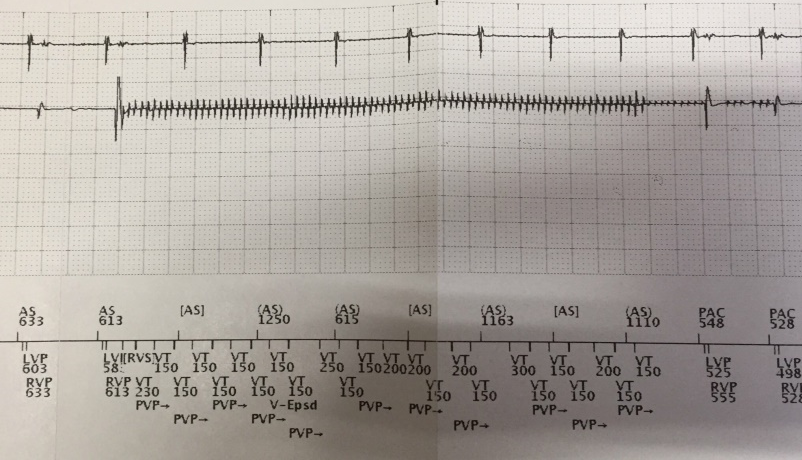

Figure 1
Stored EGM strip of a ventricular high rate episode. Top to bottom: Atrial EGM (5 mm/mV), right ventricular EGM (1 mm/mV), marker channel.

