Answer
Increase ventricular sensitivity
Explanation
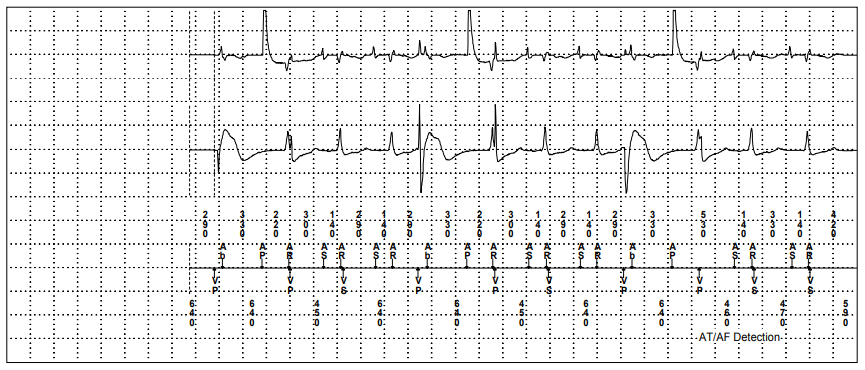
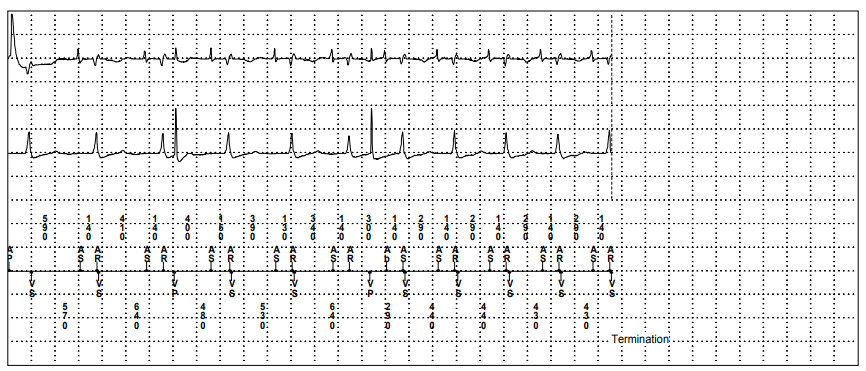
To reduce far field R wave oversensing on the atrial channel the best programming change would be to decrease the atrial sensitivity which would make it less likely to sense the far field R wave. However, this change is not the most important change to make. Figure 3 is a zoomed in section of the EGM in figure 1. Seen in the red boxes there is clear R wave undersensing with inappropriate ventricular pacing being delivered in the ventricular repolarisation period (T wave) which is known to be pro-arrhythmic and has a risk of initiating ventricular arrhythmias.
In the red boxes, the device atrially senses (AS) an atrial event. There is a deflection on the RV EGM 140 ms later which is an intrinisic R wave, this beat is undersensed as no (VS) marker is recorded. The next atrial event is a sensed far field R wave which falls in the atrial refractory period marked as an AR. As the device ventricularly undersensed the AV interval was not reset and times out at the programmed interval, 200ms. At this point the device initates a ventricular paced (VP) event and in these two examples this ventricular paced event coincides with the replorisation period. Consequently, the most important programming change required from this trace is to increase the ventricular sensitivity.
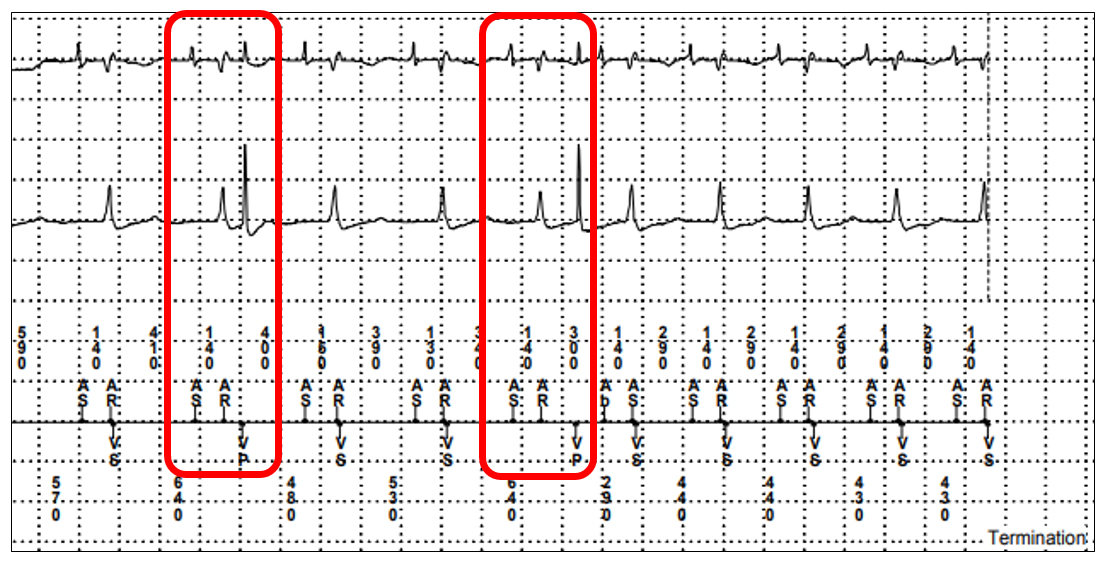
Figure 3: Ventricular Undersensing EGM. Channel 1: Atrial Bipolar EGM, Channel 2: Ventricular Bipolar EGM, Channel 3: Device Markers.
In Conclusion
In conclusion, this case highlights how it is important to review all data present in recorded EGMs when assessing for potential device malfunctions. Careful assessment of each lead, channel and the associated markers was key to identifying the two lead issues seen here. Where issues are identifed in one lead it is essential that the function of the other lead is not overlooked.