Answer
Dual tachycardia
Explanation:
Dual tachycardia is defined as an episode of atrial tachycardia or atrial fibrillation which occurs simultaneously with an episode of ventricular tachycardia. This phenomenon is uncommon and is estimated to occur in around 9% of dual-chamber ICD interrogations.1
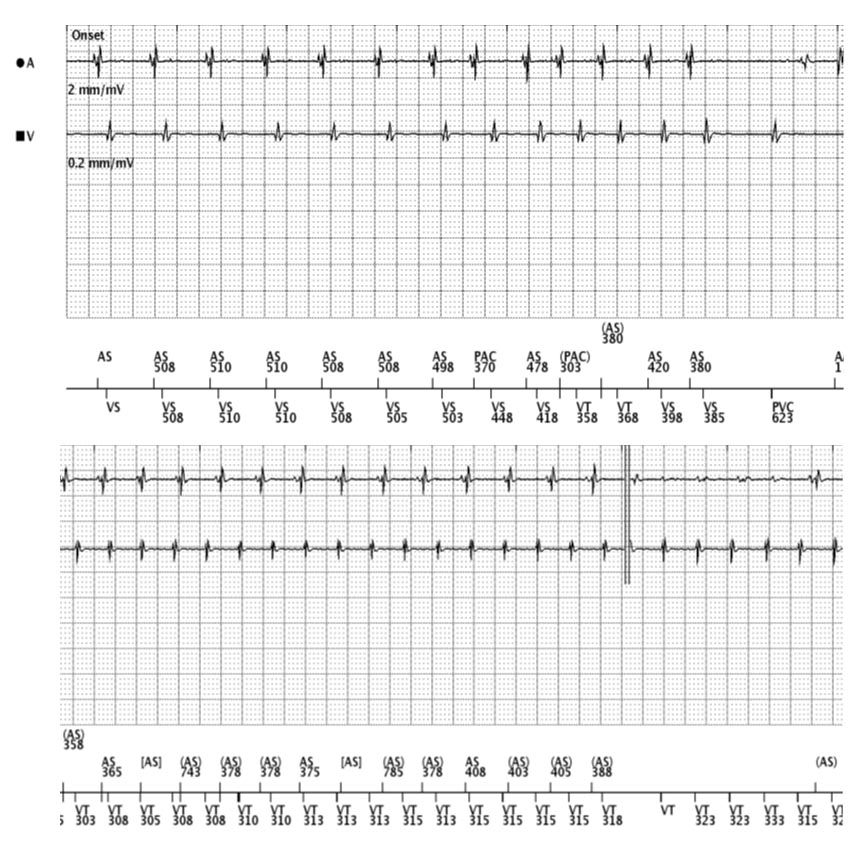
At the onset of this EGM, the rhythm is sinus tachycardia at a rate of around 120 bpm. An atrial ectopic beat (PAC) occurs on the eighth beat of the strip, resulting in a brief run of atrial tachycardia. This terminates and is followed by a ventricular ectopic beat (PVC).
The next strip shows the presence of an atrial tachycardia, with a cycle length of around 400 ms (150 bpm) and a simultaneous ventricular tachycardia with a cycle length of around 310 ms (194 bpm).
At first glance, it is easy to mistake a 1:1 AV association between the atrial and ventricular EGMs. However, upon closer inspection, it is clear that there is no true AV association due to there being inconsistent A-V intervals. The atrial and ventricular rates are also independent of one another further suggesting the presence of two independent tachycardias.
The final strip shows an ongoing ventricular tachycardia however, the atrial tachycardia appears to have terminated. The small deflections seen on the atrial channel here are likely to be small far-field ventricular signals with a clear, genuine atrial signal occurring towards the end of the strip (AS). This provides further evidence for the presence of a dual tachycardia.
Discussion:
The presence of multiple arrhythmias occurring within the same patient has been demonstrated frequently using electrophysiological studies; with multiple tachycardias demonstrating changing characteristics and emerging within a relatively short time frame in the setting of myocarditis being a specific example. However, the presence of dual atrial and ventricular tachycardias is less commonly documented with many being attributed to Digitalis toxicity. 2 However, this is not the only aetiology related to this condition and it is important to identify the arrhythmia substrate to guide the development of a treatment plan.
Studies have aimed to assess the incidence of dual tachycardia in patients receiving dual-chamber ICDs. One particular study found that dual tachycardia is more common than once believed in dual- chamber ICD recipients (8.9% of study participants) who have a history of atrial fibrillation. It was concluded that around 50% of the time, the preceding atrial tachycardia is ≤1 hour in duration and that termination of atrial fibrillation can delay the time to subsequent ventricular tachycardia detection.3
The presence of both atrial and ventricular arrhythmias in patients with cardiomyopathy is well documented and is an important factor when considering the implantation of an ICD for this subset of patients.4 In this case, it was felt likely that the severe left ventricular systolic impairment was a precipitating cause for the sustained episode of ventricular tachycardia, which had never been documented to this degree during the device follow-up of this patient. This patient was discharged with optimised pharmacological therapy for both heart failure and rate control, as well as a cardiology referral for further consideration of upgrading the patient to a dual-chamber ICD system.
References
- Li A and Epstein L. Double Trouble: Dual Tachycardia in Patient Presenting with Slow Ventricular Tachycardia, Journal of the American College of Cardiology 2020;75(11). https://doi.org/10.1016/S0735-1097(20)33319-2.
- Asirvatham S and Stevenson W. Multiple and Concurrent Arrhythmia, Circulation: Arrhythmia and Electrophysiology 2016;9(7). https://doi.org/10.1161/CIRCEP.116.003612.
- Stein K, Euler D, Mehra R, et al. Do atrial tachyarrhythmias beget ventricular tachyarrhythmias in defibrillator recipients?”, JACC 2020;40(2). https://doi.org/10.1016/S0735-1097(02)01957-5.
- Kassotis J, Haq S and Mongwa M, Multiple Cardiac Arrhythmias Detected by a Dual Chamber Implantable Cardioverter Defibrillator in a Patient with Hypertrophic Obstructive Cardiomyopathy, Hallenic Journal of Cardiology 2004;45:57-60.